 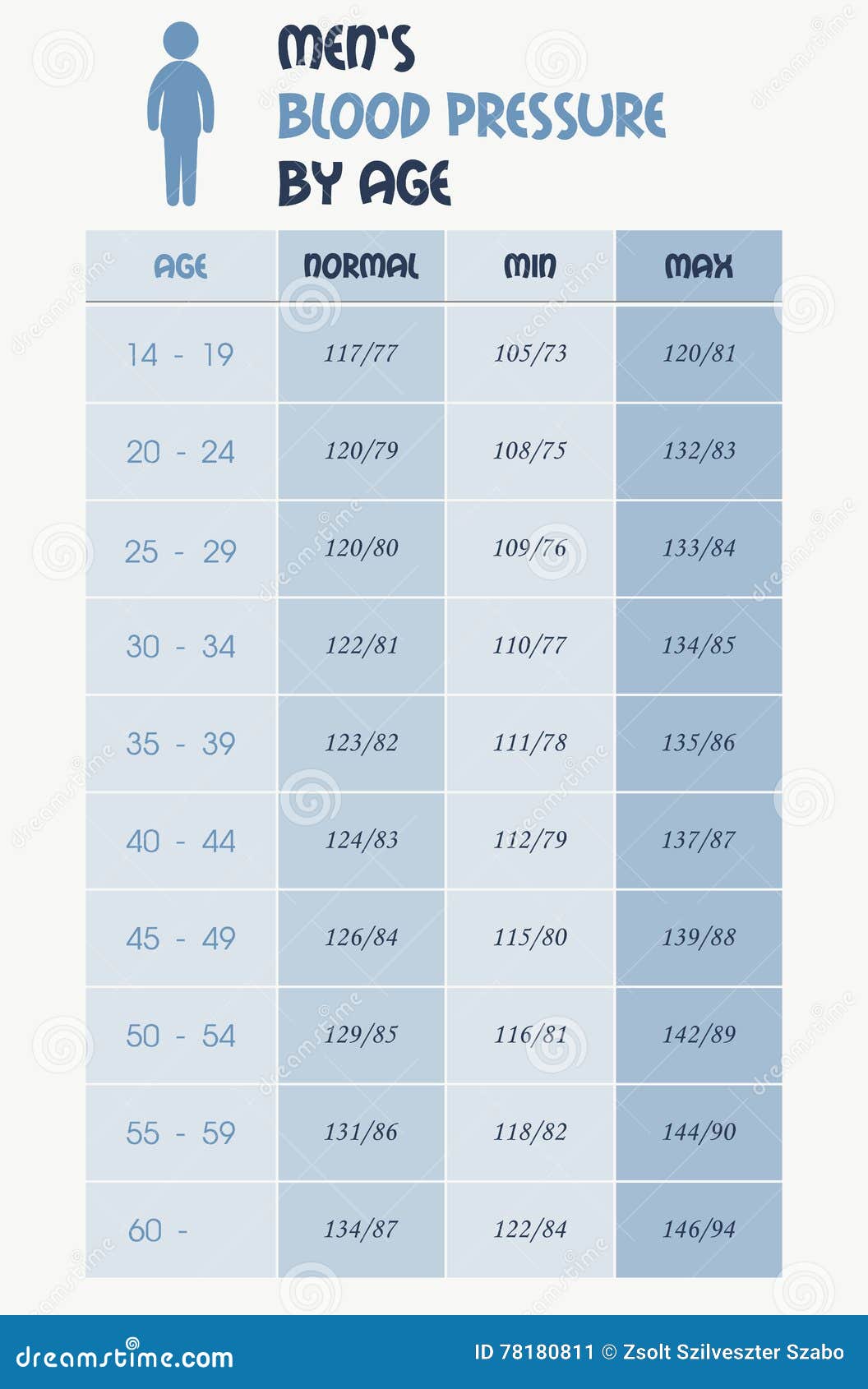
They are often under-represented in clinical trials because of other illnesses they have, treatments they are taking, limited life expectancy or dementia. But there is a lack of research into the impact of treatment in frail older people. High blood pressure is the most common disease among the over 75s. It is an important basis for further research that could improve healthcare providers' ability to provide more personalised treatment plans for older patients. But it highlights the difficulty of managing blood pressure in elderly frail patients. This research in itself will not change practice. However, there are no clear targets for the blood pressure management in frail older people. These findings are in line with the most recent 2019 NICE guidelines which recommend a higher blood pressure target, of 150mmHg, in people aged 80 years or more. The researchers found that lower than normal blood pressures were associated with a higher death rate among older people, particularly those over the age of 85 or those who were very frail. The medical records of more than 400,000 patients in primary care were reviewed. The views expressed are those of the author(s) and reviewer(s) at the time of publication.įrail older people may not benefit from the same tight blood pressure control that has been shown to benefit relatively younger, healthier groups in existing trials. Those with stronger cognitive function to begin with experienced a greater reduction in the risk of heart disease and death.Īlthough those with impaired function did not gain as much benefit, there was no indication that the lower systolic level increased their risk of heart disease or death.This is a plain English summary of an original research article. The researchers also looked at the benefits of intensive blood pressure control according to each participant’s level of cognitive function at the start of the trial. However, results showed that this level of blood pressure did not increase a person’s chances of falling. Falls often lead to complications in the elderly that can be fatal. The researchers were also concerned about the potential for falls due to very low blood pressure. People in the 120 mmHg group also saw an increased incidence of non-major, but still significant, changes to their kidney function, including hospitalizations for kidney damage. The development of dementia was about the same in both groups. The group who had achieved systolic levels of 120 mmHg or less did see a lowered risk of heart disease events, and a lower likelihood of mild cognitive impairment. To these ends, the second group received what researchers considered “intensive” treatment to bring their systolic reading down below 120 mmHg. The scientists were also interested in seeing if cognitive or physical impairments would affect the benefits of any lower systolic measurement. The researchers sought to determine if a more aggressive control of high blood pressure would benefit people’s health, lower their risk of heart disease events, cognitive decline, or death, or increase health risks in any way. The researchers randomly divided the participants into two equal groups, with one group receiving assistance in getting their systolic readings below 140 mmHg. The average baseline systolic blood pressure of the participants was approximately 142 mmHg. More than half of those included were regularly taking five or more medications. The mean age of the participants was 84, with about 3% older than 90. The majority had three or more chronic health conditions. 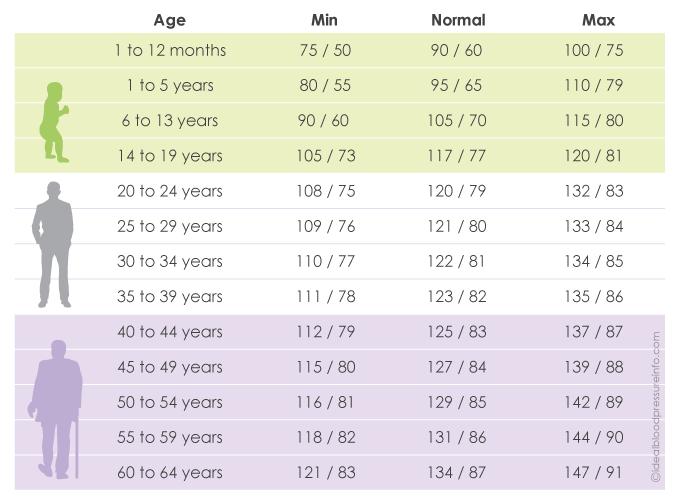
They included data from individuals who had experienced strokes, heart attacks, changes in kidney function, cognitive impairment, quality of life reduction, or who had died.Ībout 27% of them had a history of heart disease. Researchers gathered information from the Systolic Blood Pressure Intervention Trial (SPRINT). The study’s findings come from a randomized trial of 1,167 participants. Using the SPRINT study for new guidelines
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
